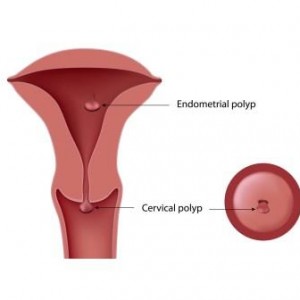
What is a Uterine Polyp?
A uterine polyp is a growth from the inside wall of your uterus into your uterine cavity. They are more common in women who are peri-menopausal or menopausal. But, they happen in younger women as well. 2 to 5% of women may experience polyps.
What causes a uterine polyp?
Research has shown a causative link between the following factors that influence the growth of polyps:
- Inflammation—Chronic inflammation causes abnormal tissue growth. Factors that cause inflammation include insulin, inflammatory foods, gut dysbiosis, hormone imbalances, and lack of exercise.
- Estrogen – Imbalanced estrogen levels also cause abnormal growth of estrogen-sensitive tissues like the uterus.
- Progesterone deficiency. Progesterone normally balances the effects of estrogen. If progesterone is reduced or absent, then estrogen goes unchecked. This causes abnormal tissue growth in the uterus.
- Ageing – As women age, ovulation occurs less often. Without ovulation, a woman cannot produce progesterone from her ovaries. Estrogen may still be made but without the protective effects of progesterone.
- Excess weight/obesity
- Unbalanced estrogen therapy
What are the symptoms of a uterine polyp?
If you have a uterine polyp, you may notice abnormal uterine bleeding or vaginal discharge. You may have bleeding between menstrual periods, particularly heavy periods, frequent periods, or have problems with infertility. If you experience these symptoms, you should see your medical doctor for investigation. After proper investigation including an ultrasound, possibly a hysteroscopy or sonohysterogram, I can help you shrink your polyps or prevent the growth of new polyps once you have the existing ones removed.
How is a uterine polyp diagnosed?
A pelvic and transvaginal ultrasound will pick up polyps. Your doctor may also order a hysteroscopy or sonohysterogram.
What is the treatment for polyps?
Medical doctors recommend surgery to remove polyps in most instances.
What is the natural treatment for polyps in the uterus?
To naturally shrink cervical or endometrial polyps, we need to address all the factors contributing to them. Whether they will respond to naturopathy depends on the size and cause of the polyps.
Address the root cause
Estrogen dominance will cause polyps. This is where there is an imbalance between your levels of estrogen and progesterone, the two main female hormones. To correct this, we reduce the excessive estrogen production by cleaning up your diet. We help your liver remove any excess estrogen and support healthy progesterone production. Under stress, you may not ovulate. In this case, you can’t make progesterone on a given cycle. Stress management can help preserve your progesterone.
Inflammation
There are a number of factors that provoke, aggravate, or create inflammation in your body. These include:
- Food sensitivities
- Insulin
- Poor diet
- Latent infection
- Chemicals
- Hormone imbalance
- Heavy metals
- Mold exposure
All of these are improved through naturopathic treatment.
Food sensitivities
Low-grade allergies to foods contribute to inflammation in the body. This inflammation can be widespread and not limited to the digestive tract. However, it can also show up as digestive problems like constipation, diarrhea, acid reflux, GERD, bloating, gas, and nausea.
Insulin
When you eat foods that increase your blood sugar level, your insulin levels increase to bring the blood sugar level down. Insulin promotes inflammation and abnormal tissue growth. Research shows an association between insulin resistance and endometrial (uterine) polyps.
Poor diet
Certain foods are pro-inflammatory, while others are anti-inflammatory. For example, trans fats are more inflammatory, while fish oils are anti-inflammatory. Some foods provoke the release of much more insulin than others. An anti-inflammatory, low-carb diet may help.
Latent infection
A latent infection is one that you may not be aware of. The symptoms are mild enough that you may not notice them. However, these low-grade infections can perpetuate inflammation of the cervix and contribute to polyp development.
Estrogen
For women, estrogen is necessary to build a uterine or endometrial lining. It is produced as an egg follicle is developing each month. However, excess estrogen, chemicals that act like estrogen or estrogen that is not well-balanced by other hormones, causes problems like polyps. How does this happen?
Excess estrogen
Once your body has enough estrogen, your liver must process and break down the extra for removal. What ingredients are needed for this process? Vitamin B6, vitamin B12, magnesium, 5MTHF, indole-3-carbinol, sulfur, and glucaric acid (glucarate). If your body is missing one or more of these ingredients, estrogen may not be fully processed into waste. So, it isn’t excreted. Will a blood test for estrogen show this? No. Blood tests don’t measure many of the different forms of estrogen, such as estrone and estriol. Supplements for uterine polyps include vitamin B6, B12, magnesium, L-5MTHF, I3C, and glucarate to support healthy liver removal of estrogen and estrogen-like compounds, like BPA from plastic.
Excessive estrogen production or activity
Carbs and sugar in your diet increase your blood levels of insulin. Higher insulin, then, drives increased production of estrogen. Insulin also lowers levels of Sex Hormone Binding Globulin (SHBG). SHBG helps control estrogen activity. So, lowering SHBG increases estrogen activity.
Lack of hormones that should be balancing estrogen
Progesterone, testosterone, DHEAs, and androstenedione all balance estrogen by competing with it for receptor sites. Low levels of these hormones happen because of excessive stress. Through a feedback loop, high levels of estrogen can suppress their production. Lack of specific vitamins and minerals, such as vitamin B6, negatively affects hormone production and metabolism. Women with other conditions that are indicative of hormonal imbalance, such as endometriosis and PCOS may be at greater risk of developing polyps.
Should you treat a uterine polyp?
Yes. Even if polyps are surgically removed, the underlying cause of the polyps still remains. Naturopathic treatment of polyps in the uterus addresses the cause and prevents polyp regrowth after surgery.
Polyps in Postmenopausal Women
12% of postmenopausal women over the age of 59 with abnormal uterine bleeding will have malignant lesions. Surgical removal is recommended.
For help with this or any other health problem, book an appointment here or call the clinic for more information at 416-481-0222. I can give you tailored advice in person or virtually if you are anywhere in Ontario. If you are elsewhere, I can’t provide personalized treatment, but you can get general information about natural approaches for PCOS-related polyps in my ebook here.
by Dr Pamela Frank, BSc(Hons), ND
Uterine Polyp Research
Eur J Obstet Gynecol Reprod Biol. 2017 Sep;216:138-142. doi: 10.1016/j.ejogrb.2017.07.013. Epub 2017 Jul 15.
Risk of malignancy on suspicion of polyps in menopausal women.
Bel S, Billard C, Godet J, Viviani V, Akladios C, Host A, Faller E, Boisrame T, Hummel M, Baldauf JJ, Lecointre L, Garbin O.
J Clin Endocrinol Metab. 1994 Oct;79(4):1173-6.
The relationship between serum levels of insulin and sex hormone-binding globulin in men: the effect of weight loss. Strain G1, Zumoff B, Rosner W, Pi-Sunyer X.
Georgian Med News. 2017 Dec;(273):16-22.
ENDOMETRIAL POLYPS IN WOMEN OF REPRODUCTIVE AGE: CLINICAL AND PATHOGENETIC VARIATIONS. Kosei N1, Zakharenko N1, Herman D1.
Özkan NT, Tokmak A, Güzel Aİ, Özkan S, çİçek MN. The association between endometrial polyps and metabolic syndrome: a case-control study. Aust N Z J Obstet Gynaecol. 2015 Jun;55(3):274-8. doi: 10.1111/ajo.12339. Epub 2015 Jun 5. PMID: 26044674.
Alkilani YG, Apodaca-Ramos I. Cervical Polyps. [Updated 2021 Sep 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562185/
Dr. Pamela Frank has been in practice as a naturopathic doctor for over 26 years. Since 1999, she has earned acclaim as a leading naturopath in Toronto, amassing multiple awards.
Dr. Pamela has a special interest in addressing hormone-related complexities, including but not limited to PCOS, endometriosis, acne, hair loss, weight management, thyroid issues, and fertility.
Residing in Toronto with her family and loyal companion, Dolly the rescue dog, Dr. Pamela seamlessly combines her professional commitment with a diverse range of interests.
Beyond her clinical endeavours, she actively engages in kickboxing, leadership roles within Scout Groups, yoga practice, podcasting, and outdoor pursuits such as backcountry camping.
Dr. Pamela’s comprehensive approach reflects not only her dedication to optimal health but also her passion for continual personal and professional growth.
